Chinese Journal of Tissue Engineering Research ›› 2014, Vol. 18 ›› Issue (40): 6476-6481.doi: 10.3969/j.issn.2095-4344.2014.40.014
Previous Articles Next Articles
Early effect of lumbar dynamic fixation for treatment of lumbar disc herniation
Ming Jiang-hua1, Zhao Qi1, Yang Bin2, Zheng Hui-feng1
- 1 Department of Orthopedics, Renmin Hospital of Wuhan University, Wuhan 430060, Hubei Province, China;2 Yangxin County People’s Hospital, Yangxin 435200, Hubei Province, China
-
Revised:2014-07-24Online:2014-09-24Published:2014-09-24 -
About author:Ming Jiang-hua, Chief physician, Master’s supervisor, Department of Orthopedics, Renmin Hospital of Wuhan University, Wuhan 430060, Hubei Province, China Zhao Qi, Department of Orthopedics, Renmin Hospital of Wuhan University, Wuhan 430060, Hubei Province, China Ming Jiang-hua and Zhao Qi contributed equally to this paper.
CLC Number:
Cite this article
Ming Jiang-hua, Zhao Qi, Yang Bin, Zheng Hui-feng. Early effect of lumbar dynamic fixation for treatment of lumbar disc herniation[J]. Chinese Journal of Tissue Engineering Research, 2014, 18(40): 6476-6481.
share this article
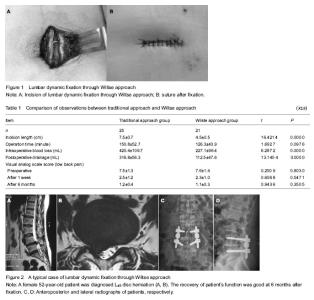
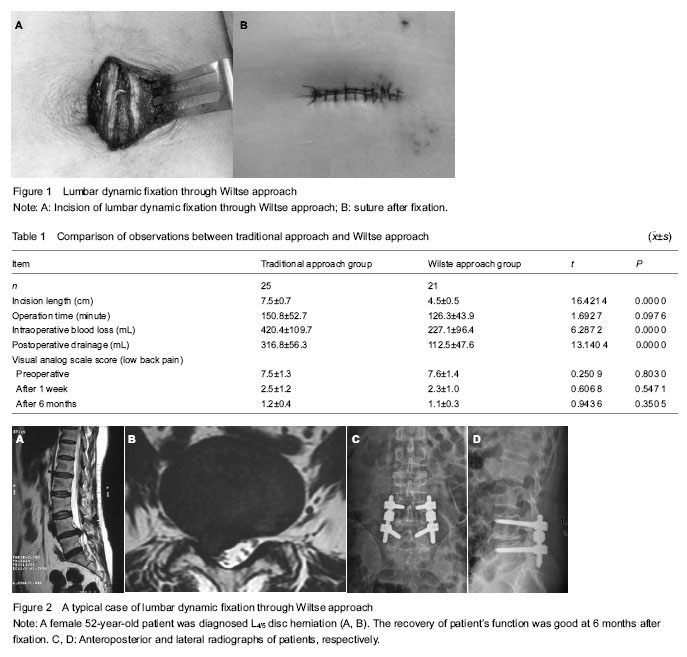
Quantitative analysis of subjects All participants were included in the final analysis. The groups of 46 patients were followed up for 7 to 31 months, mean 13.8 ± 2.4 months. Effects of lumbar dynamic fixation through Wiltse approach Two groups of patients at 1 week after low back pain were significantly reduced, and the difference between the visual analog scale score before surgery was statistically significant (P=0.000 0). Compared to the length of the incision, the differences in intraoperative blood loss and postoperative drainage were statistically significant between two groups of patients, while no significant difference in the operation of low back pain visual analog scale score and time after 1 week and after 6 months was found (P > 0.05; Table 1). Adverse reactions of lumbar dynamic fixation through Wiltse approach Four patients wound suffer from effusion postoperative and delayed healing after puncture with bandaged in traditional approach group, and the remaining wounds healed. In Wilste approach group, two patients had partial necrosis of the skin incision edge, after dressing healed. At the final follow-up, X-ray showed a good fixation position and no loose or broken in all patients. Typical case of lumbar dynamic fixation through Wiltse approach There was a typical case, female, aged 52, L4/5 disc herniation with right lower extremity pain and numbness for three months (Figure 2)."
| [1] Verdú-López F, Beisse R. Current status of thoracoscopic surgery for thoracic and lumbar spine. Part 2: treatment of the thoracic disc hernia, spinal deformities, spinal tumors, infections and miscellaneous. Neurocirugia (Astur). 2014;25(2):62-72.
[2] Manchikanti L, Abdi S, Atluri S, et al. An update of comprehensive evidence-based guidelines for interventional techniques in chronic spinal pain. Part II: guidance and recommendations. Pain Physician. 2013;16(2 Suppl):S49-283.
[3] Kotil K, Köksal NS, Kayaci S. Long term results of lumbar sequestrectomy versus aggressive microdiscectomy. J Clin Neurosci. 2014, in press.
[4] Nie H, Hao J, Peng C, et al. Clinical outcomes of discectomy in octogenarian patients with lumbar disc herniation. J Spinal Disord Tech. 2013;26(2):74-78.
[5] Disch AC, Schmoelz W, Matziolis G, et al. Higher risk of adjacent segment degeneration after floating fusions: long-term outcome after low lumbar spine fusions. J Spinal Disord Tech. 2008;21(2):79-85.
[6] Ghiselli G, Wang JC, Bhatia NN, et al. Adjacent segment degeneration in the lumbar spine. J Bone Joint Surg Am. 2004;86-A(7):1497-1503.
[7] Maida G, Altruda C, Gatti M, et al. Two-year follow-up after microsurgical di-scectomy and dynamic percutaneous stabilization in degenerate and herniated lumbar disc: clinical and neuroradiological outcome. J Neurosurg Sci. 2014;58(2):95-102.
[8] Xu D, Xu HZ, Chen YH, et al. Discectomy and discectomy plus Coflex fixation for lumbar disc herniation, a clinical comparison study. Zhonghua Wai Ke Za Zhi. 2013;51(2): 147-151.
[9] Huang KF, Chen TY. Clinical results of a single central interbody fusion cage and transpedicle screws fixation for recurrent herniated lumbar disc and low-grade spondylolisthesis. Chang Gung Med J. 2003;26(3):170-177.
[10] Häkkinen A, Kuukkanen T, Tarvainen U, et al. Trunk muscle strength in flexion, extension, and axial rotation in patients managed with lumbar disc herniation surgery and in healthy control subjects. Spine (Phila Pa 1976). 2003;28(10):1068- 1073.
[11] Bokov A, Isrelov A, Skorodumov A, et al. An analysis of reasons for failed back surgery syndrome and partial results after different types of surgical lumbar nerve root decompression. Pain Physician. 2011;14(6):545-557.
[12] Ruetten S, Komp M, Merk H, et al. Recurrent lumbar disc herniation after conventional discectomy: a prospective, randomized study comparing full-endoscopic interlaminar and transforaminal versus microsurgical revision. J Spinal Disord Tech. 2009;22(2):122-129.
[13] Parker SL, Godil SS, Mendenhall SK, et al. Two-year comprehensive medical management of degenerative lumbar spine disease (lumbar spondylolisthesis, stenosis, or disc herniation): a value analysis of cost, pain, disability, and quality of life. J Neurosurg Spine. 2014, in press.
[14] Cueva-del Castillo Mendoza JF, Franco-López EA, Hinojosa- Sandoval F, et al. Lumbar herniated disks treated with a dynamic interspacer. Acta Ortop Mex. 2013;27(2):87-91.
[15] Yu PF, Jiang FD, Liu JT, et al. Outcomes of conservative treatment for ruptured lumbar disc herniation. Acta Orthop Belg. 2013;79(6):726-730.
[16] Jacobs WC, Rubinstein SM, Koes B, et al. Evidence for surgery in degenerative lumbar spine disorders. Best Pract Res Clin Rheumatol. 2013;27(5):673-684.
[17] Manchikanti L, Singh V, Falco FJ, et al. An updated review of automated percutaneous mechanical lumbar discectomy for the contained herniated lumbar disc. Pain Physician. 2013;16(2 Suppl):SE151-184.
[18] Adam D, Pevzner E, Gepstein R. Comparison of percutaneous nucleoplasty and open discectomy in patients with lumbar disc protrusions. Chirurgia (Bucur). 2013; 108(1):94-98.
[19] Lee GW, Lee SM, Suh BG. The impact of generalized joint laxity on the occurrence and disease course of primary lumbar disc herniation. Spine J. 2014, in press.
[20] Niesche M, Juratli TA, Sitoci KH, et al. Percutaneous pedicle screw and rod fixation with TLIF in a series of 14 patients with recurrent lumbar disc herniation. Clin Neurol Neurosurg. 2014;124C:25-31.
[21] Grotle M, Solberg T, Storheim K, et al. Public and private health service in Norway: a comparison of patient characteristics and surgery criteria for patients with nerve root affections due to discus herniation. Eur Spine J. 2014, in press.
[22] Park JS, Choi SE, Cho TK, et al. Recurrence rate after herniotomy only versus discectomy in lumbar disc herniation. Korean J Spine. 2013;10(4):227-231.
[23] Li Y, Fredrickson V, Resnick DK. How should we grade lumbar disc herniation and nerve root compression? A systematic review. Clin Orthop Relat Res. 2014, in press.
[24] Mroz TE, Lubelski D, Williams SK, et al. Differences in the surgical treatment of recurrent lumbar disc herniation among spine surgeons in the United States. Spine J. 2014, in press.
[25] Kubaszewski L, Kaczmarczyk J, Nowakowski A, et al. Foraminoplastic transfacet epidural endoscopic approach for removal of intraforaminal disc herniation at the L5-S1 level. Wideochir Inne Tech Malo Inwazyjne. 2014;9(1): 96-100.
[26] Huang CJ, Tang HW, Liang DB, et al. Treatment of the recurrent lumbar disc herniation:a comparison between endoscopic surgery and open surgery. Zhongguo Gu Shang. 2013;26(10):810-814.
[27] Xin G, Shi-Sheng H, Hai-Long Z. Morphometric analysis of the YESS and TESSYS techniques of percutaneous transforaminal endoscopic lumbar discectomy. Clin Anat. 2013;26(6):728-734.
[28] Wu H, Yu WD, Jiang R, et al. Treatment of multilevel degenerative lumbar spinal stenosis with spondylolisthesis using a combination of microendoscopic discectomy and minimally invasive transforaminal lumbar interbody fusion. Exp Ther Med. 2013;5(2):567-571.
[29] Cho KS, Kang SG, Yoo DS, et al. Risk factors and surgical treatment for symptomatic adjacent segment degeneration after lumbar spine fusion. J Korean Neurosurg Soc. 2009;46(5):425-430.
[30] Wang JC, Dailey AT, Mummaneni PV, et al. Guideline update for the performance of fusion procedures for degenerative disease of the lumbar spine. Part 8: Lumbar fusion for disc herniation and radiculopathy. J Neurosurg Spine. 2014;21(1):48-53.
[31] Zeng ZY, Zhang JQ, Song YX, et al. Combination of percutaneous unilateral translaminar facet screw fixation and interbody fusion for treatment of lower lumbar vertebra diseases: a follow-up study. Orthop Surg. 2014;6(2): 110-117.
[32] Zhao D, Deng SC, Ma Y, et al. Surgical options and clinical outcomes in patients of lumbar disc herniation with Modic changes. Zhonghua Yi Xue Za Zhi. 2013;93(39):3111-3115.
[33] Du FT. Clinical analysis of interspinous dynamic internal fixation with the Coflex system in treating lumbar degenerative disease. Zhongguo Gu Shang. 2011;24(4): 291-294.
[34] DePalma MJ, Ketchum JM, Saullo TR. Etiology of chronic low back pain in patients having undergone lumbar fusion. Pain Med. 2011;12(5):732-739.
[35] Liu M, Kan W, Li P, et al. Effectiveness of discectomy combined with Isobar non-fusion internal fixation in treating lumbar disc protrusion. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2011;25(2):229-234.
[36] Liu B, Yin D, Wang QM, et al. Lumbar interspinous non-fusion techniques: comparison between Coflex™ and Wallis. Nan Fang Yi Ke Da Xue Xue Bao. 2010;30(11): 2455-2458.
[37] Chen H, Ding W. Research advancement of lumbar inter-spinous process non-fusion techniques. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2010;24(3):368-373.
[38] Mulholland RC, Sengupta DK. Rationale, principles and experimental evaluation of the concept of soft stabilization. Eur Spine J. 2002;11 Suppl 2:S198-205.
[39] Liu C, Wang L, Tian JW. Early clinical effects of the Dynesys system plus transfacet decompression through the Wiltse approach for the treatment of lumbar degenerative diseases. Med Sci Monit. 2014;20:853-859.
[40] Chien CY, Kuo YJ, Lin SC, et al. Kinematic and Mechanical Comparisons of Lumbar Hybrid Fixation using Dynesys and Cosmic Systems. Spine (Phila Pa 1976). 2014, in press.
[41] Segura-Trepichio M, Ferrández-Sempere D, López-Prats F, et al. Pedicular dynamic stabilization system. Functional outcomes and implant-related complications for the treatment of degenerative lumbar disc disease with a minimum follow-up of 4 years. Rev Esp Cir Ortop Traumatol. 2014;58(2):85-91.
[42] von Strempel A. Dynamic posterior stabilization with the cosmic system. Oper Orthop Traumatol. 2010;22(5-6): 561-572.
[43] Stoffel M, Behr M, Reinke A, et al. Pedicle screw-based dynamic stabilization of the thoracolumbar spine with the Cosmic-system: a prospective observation. Acta Neurochir (Wien). 2010;152(5):835-843.
[44] Ferreux L, Moutard G, Branger T. Measurement of natural radionuclides in phosphgypsum using an anti-cosmic gamma-ray spectrometer. Appl Radiat Isot. 2009;67(5): 957-960.
[45] Schmoelz W, Huber JF, Nydegger T, et al. Dynamic stabilization of the lumbar spine and its effects on adjacent segments: an in vitro experiment. J Spinal Disord Tech. 2003; 16(4):418-423.
[46] Stoll TM, Dubois G, Schwarzenbach O. The dynamic neutralization system for the spine: a multi-center study of a novel non-fusion system. Eur Spine J. 2002;11 Suppl 2: S170-178.
[47] Erbulut DU, Kiapour A, Oktenoglu T, et al. A computational biomechanical investigation of posterior dynamic instrumentation: combination of dynamic rod and hinged (dynamic) screw. J Biomech Eng. 2014;136(5):051007.
[48] Schwarzenbach O, Berlemann U. Dynamic posterior stabilization with the pedicle screw system DYNESYS®. Oper Orthop Traumatol. 2010;22(5-6):545-557.
[49] Stevens KJ, Spenciner DB, Griffiths KL, et al. Comparison of minimally invasive and conventional open posterolateral lumbar fusion using magnetic resonance imaging and retraction pressure studies. J Spinal Disord Tech. 2006; 19(2):77-86.
[50] Kim KT, Lee SH, Suk KS, et al. The quantitative analysis of tissue injury markers after mini-open lumbar fusion. Spine (Phila Pa 1976). 2006;31(6):712-716.
[51] Boelderl A, Daniaux H, Kathrein A, et al. Danger of damaging the medial branches of the posterior rami of spinal nerves during a dorsomedian approach to the spine. Clin Anat. 2002;15(2):77-81.
[52] Wiltse LL, Bateman JG, Hutchinson RH, et al. The paraspinal sacrospinalis-splitting approach to the lumbar spine. J Bone Joint Surg Am. 1968;50(5):919-926.
[53] Buttermann GR, Mullin WJ. Two-level circumferential lumbar fusion comparing midline and paraspinal posterior approach: 5-year interim outcomes of a randomized, blinded, prospective study. J Spinal Disord Tech. 2013, in press. |
| [1] | Fang Yi, Zhao Wenzhi, Pan Deyue, Han Xin, Zhang Lu, He Hongtao, Shi Feng, Tian Tingxiao. Acromioclavicular joint dislocation: how to achieve anatomical reduction, sustained stability and micro-motion [J]. Chinese Journal of Tissue Engineering Research, 2020, 24(5): 796-802. |
| [2] | Fu Jiaxin, Xiao Lianping, Wang Shusen, Li Xiaodong, Han Liqiang, Wang Tonghao. Therapeutic effects of paraspinal approach combined with internal fixation through pedicle of fractured vertebra versus traditional AF screw-rod system for thoracolumbar fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1177-1181. |
| [3] | Qiu Zhongpeng, Li Ke, Li Gang, Liu Keyu, Du Xinhui, Meng Defeng, Shi Chenhui, Wang Weishan. Different treatments for two-part and three-part proximal humeral fractures by Neer classification: follow-up results analyzed using clinical economics [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1188-1195. |
| [4] | Ke Wei, Li Ke, Wang Sibo, Du Xinhui, Qiu Zhongpeng, Kang Zhilin, Wang Weishan, Li Gang . Open reduction and plate fixation versus closed reduction and external fixation for distal radius fractures: scores and linear regression analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1196-1202. |
| [5] | Shu Gao, Chen Xiaodong, Zhai Mingyu, Li Quanxiu, Liang Pengzhan, Yang Xuejun, Zhao Haibo, Yu Chenqiang, Bai Xueling, Li Long. Imaging evaluation and biomechanical characteristics of the novel intradiscal electrothermal annuloplasty in pigs [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1214-1221. |
| [6] | Fan Zhirong, Peng Jiajie, Zhong Degui, Zhou Lin, Su Haitao, Huang Yongquan, Wu Jianglin, Liang Yihao. Suture anchor combined with open reduction and internal fixation versus open reduction and internal fixation for ankle fracture combined with deltoid ligament injury: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(8): 1307-1312. |
| [7] | Zhou Yu, Liu Yuehong, Liu Shuping, Chen Xi, Qin Wei, Li Qifeng. Spinal stability of intervertebral grafting reinforced by five or six augmenting screws versus transvertebral grafting reinforced by four augmenting screws for thoracolumbar vertebral fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 505-511. |
| [8] | Li Xianzhou, Wang Qian, Zhang Cunxin . Lumbar spondylolisthesis: status and prospects of implant treatment [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(4): 621-627. |
| [9] | Yin Hao, Zhou Enchang, Pan Zhengjun, Chen Guang, Jiang Hua. Finite element analysis of the four and three cannulated screws combined with buttress plate fixation for the treatment of Pauwels III femoral neck fractures [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(32): 5133-5137. |
| [10] |
Wang Lei, Li Zilong, Yuan Binbin, Wu Qingwei, Tang Fengming.
Clinical effect of locking plate versus anterograde intramedullary nail in the treatment of adult humeral shaft fractures: a meta-analysis
[J]. Chinese Journal of Tissue Engineering Research, 2019, 23(24): 3924-3930.
|
| [11] | Li Pengfei, Wang Tao, Ma Xinlong . Association between COL9A2 gene polymorphisms and intervertebral disc degeneration in Asian: a meta-analysis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(20): 3275-3280. |
| [12] | Hao Liang, Zhang Zhonglin, Wang Baodong, Bi Zhenggang. Intertrochanteric fracture of the femur: improvement of internal fixation device, surgical changes and related disputes [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(18): 2927-2935. |
| [13] | Yao Liquan, Ling Qinjie, Li Jiaying, Zhong Letian, Zhou Xingping, Liu Jintao, He Erxing, Yin Zhixun. Antibiotic artificial bone implantation for treating pyogenic spondylodiscitis [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(14): 2133-2139. |
| [14] | Gong Zhibing, Wu Zhaoke, Zhang Huantang, Xu Zhiqing, Zhuang Zhikun, Zhang Qianjin. Allogeneic cortical bone plate combined with locking plate for Vancouver type B1 and C osteoporotic periprosthetic femoral fractures after hip arthroplasty in older adults [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1812-1817. |
| [15] | Li Xiaofeng, Xie Furong, Zhan Long, Yang Yuan. Design of locking compression plate through transoral approach [J]. Chinese Journal of Tissue Engineering Research, 2019, 23(12): 1824-1828. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||